
‘The only truly political action is that which severs the nexus between violence and law.’
— Giorgio Agamben, State of Exception
Table of Contents
- Government Guidance and the Law
- Benefits and Dangers of Wearing Masks
- Asymptomatic Transmission of Coronavirus
- Surveillance and Compliance
- Civil Disobedience
Appendix: Medical Advice against Wearing Masks
Addendum 1. New Regulations on Wearing Masks on Public Transport
Addendum 2. Further Regulations on Wearing Masks in Shops and Other Places
Addendum 3. Psychological Impact of Wearing Masks on School Children
Postscript. Summary of Amendments to the Coronavirus-justified Regulations on Wearing Face Coverings
This article was first published on 11 June, when advice on wearing masks was restricted to Government Guidance and had no legal force. On 15 June the article was updated in response to The Health Protection (Coronavirus, Wearing of Face Coverings on Public Transport) (England) Regulations 2020, which are analysed in Addendum 1. On 24 July it was updated again in response to The Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) Regulations 2020, the analysis of which can be found in Addendum 2. Subsequent changes to Government regulations on the mandatory wearing of masks can be found in the postscript. The science on their lack of efficacy in stopping viral transmission and the dangers they present to the health of the wearer remains the same.
1. Government Guidance and the Law
On 30 March, former Supreme Court Justice Jonathan Sumption, QC, in a widely-reported condemnation of the abuse of legal regulations by UK police forces in enforcing Government guidance on social distancing, reminded the British people that:
‘Policemen are citizens in uniform. They are not members of a disciplined hierarchy operating just at the Government’s command. The police have no power to enforce Ministers’ preferences, but only legal regulations, which don’t go anything like as far as the Government’s guidance. This is what a police state is like. It’s a state in which the Government can issue orders or express preferences with no legal authority and the police will enforce Ministers’ wishes.’
Two-and-a-half months later, it is time to remind ourselves that, despite the announcement last week by the Secretary of State for Transport that from 15 June the wearing of face masks on public transport will be ‘mandatory’, there is currently nothing in existing legislation, neither the Coronavirus Act 2020 nor the Health Protection (Coronavirus, Restrictions) (England) Regulations 2020, that empowers a police officer to compel a UK citizen to wear a mask on public transport.*
(*For the new Government legislation coming into effect on 15 June and 24 July, see the Addenda at the end of this article.)
Relying on the mass compliance of the British public to the extralegal imposition of these measures, both the Secretary of State and the the Chairman of Network Rail have said that British Transport police will enforce these Government guidelines. However, on 4 June, BTP issued the following statement clarifying its powers in relation to this lastest attempt to violate our civil liberties:
‘BTP has no powers regarding the National Rail Conditions of Travel, which is a contract between the train operators and the passenger travelling. If a passenger does not comply with the conditions set, the train company can refuse entry onto the service. If our officers encounter passengers not wearing a face covering on the network, they will engage with passengers and encourage them to comply with the National Rail Conditions of Travel.’
At present, therefore, the Government has said it is relying on the National Rail Conditions of Travel and Public Service Vehicle Regulations for buses. However, in London, the most up-to-date Conditions of Carriage — Bus and Underground Services published by Transport for London and valid from 20 April 2020 until further notice, make no mention of the compulsory wearing of masks. And as Jonathan Sumption, QC, would no doubt remind both us and British Transport staff, it is by these conditions, and not the preferences of Ministers or the guidelines of Government, that TfL can — and indeed must — refuse or grant access to what is a public service:
‘These Conditions of Carriage, which may be amended from time to time, replace all previous versions published by TfL and its predecessors. They come into force from the date shown on the front and will remain in force, with any amendments that we may make from time to time, until we republish them. The most up-to-date version is available at tfl.gov.uk/terms. Our staff and agents have no authority to make individual exceptions to these Conditions of Carriage.’
At present, therefore, there is neither a legal nor a contractual basis to enforcing the wearing of masks as a condition of travel on public transport in England.* And even if the Government rushes through an amendment to existing legislation by 15 June (and since publishing this article the Government has promised new Regulations made under the Public Health (Control of Disease) Act 1984 and coming into force on Monday, with disobedience punishable by a £100 fine), emergency measures in violation of our human rights and civil liberties need to be ‘justified’ and ‘proportionate’ in order to be legal, and removing the public’s access to public transport is neither.
(*On 15 June, Transport for London published new Conditions of Carriage in line with the Government’s new Regulations on face coverings.)
2. Benefits and Dangers of Wearing Masks
There are few issues about which the medical profession — which throughout this crisis we have seen subject to external political and financial pressures — is so divided*; but an overwhelming mass of medical and scientific opinion is not only that masks do nothing to stop the spread of SARs-COV-2, but that non-medical masks of the type we are being advised to wear on public transport by the Government — a supposedly life-saving device it recommends fashioning from an old T-shirt — can endanger the wearer by increasing the chance of infection: either through a build-up of the exhaled virus on the inside of the damp cloth covering; or by increasing the incidence of hand-to-face contact while fitting, adjusting and removing the covering. By restricting the wearer’s intake of oxygen, face coverings may — again, the evidence is inconclusive either way — cause headaches, dizziness, shortness of breath or worse. Making such guidance mandatory, therefore, may be in contravention of Article 1 of the Human Rights Act 1998: ‘Everyone’s right to life shall be protected by law.’ Given the widespread association of face coverings with subservience, both historically on prisoners and slaves and in contemporary cultures, it may also violate Article 3: ‘No one shall be subjected to degrading treatment’. And, given the weight of evidence of the political motivation for making face-coverings mandatory, and in the absence of conclusive scientific proof supporting this decision, it may also violate Article 14: ‘Enjoyment of rights and freedoms without discrimination on grounds of political opinion’.
As an example of the political pressures on the medical profession to give scientific credence to politically-motivated decisions, on 1 June, The Lancet published ‘Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis’. A review of 172 studies, this concluded that medical masks ‘might result in’, and N95 respirators ‘might be associated with’, a reduction in virus; yet concludes that this is evidence for advocating Government regulations for home-made masks, about which its review says nothing. Then on 5 June the World Health Organisation promptly revised its ‘Advice on the use of masks in the context of COVID-19’. However, this revision relates primarily to all health workers now being advised to wear medical masks, which will put an even greater burden on production of PPE in the UK. With regard to the rest of us wearing hand-made masks, their advice has changed little. The WHO clearly states that there is still no evidence for the effectiveness of non-medical masks. The list of reasons they give for wearing one are social rather than medical, including ‘making people feel they can play a role in contributing to stopping spread of the virus’ and, more significantly, ‘reminding people to be compliant with other measures’ and ‘encouraging public acceptance of protection measures in general’. Against which, the WHO has a long list of potential harms and dangers from such masks, which you can read about in the appendix, and which are primarily concerns about the increased risk of infection from hand-made masks. But their conclusion is very clear: ‘A non-medical mask is neither a medical device nor personal protective equipment.’
In fact, the only medical benefit — and even that is only a ‘likely advantage’ — of the use of masks by healthy people in the general public listed by the WHO is the ‘reduced potential exposure risk from infected persons before they develop symptoms.’ It’s important to clarify that this is a risk that I take, not that I represent, of potential exposure to infection from someone else who, presumably, has COVID-19 and breathes, sneezes or coughs on me in sufficiently close proximity for airborne particles or tiny droplets potentially carrying the virus to enter my nose, mouth or eyes. However, if I want to take that risk of potential exposure, that’s up to me, just as I also risk being run down by a car when I cross the road. It’s not the role of the police — and it most certainly isn’t within their legal powers — to compel me to avoid that risk. That’s my right, without which any and every possible or putative risk to my or anyone else’s safety can be used to justify controlling every aspect of my life.
If I have COVID-19, then, yes, I pose a small risk to people over 65 with one or more pre-existing co-morbidities, so I would accept not travelling on public transport at times when I might come into sufficiently close contact with such a person to spread the disease, for instance at rush hour, just as I try to avoid such a scenario when I have influenza. Rationally, it would make far more sense for the far smaller percentage of the UK population at risk of death from COVID-19 not to travel on public transport at such a time; but again, that risk is up to them to decide, not the Government. But unless I constitute a clear and present danger to those around me, there is no reason — and the WHO offers no clear medical advice or evidence to the contrary — for me to wear a hand-made mask on public transport.
3. Asymptomatic Transmission of Coronavirus
The response to this argument for civil liberties is that I do not know whether I constitute a threat, and that, as a possibly asymptomatic or pre-symptomatic carrier of SARs-CoV-2, I can unwittingly infect others by coughing or sneezing over them. The response to this is twofold. The first is that I take the same risk from using public transport with others who may also be unknowingly infected, and, once again, it is my risk to take, not the Government’s decision to impose on me intrusive, untested and possibly medically dangerous measures to eradicate that risk. And the second is that there is no conclusive evidence that asymptomatic or pre-symptomatic persons infected with SARs-CoV-2 can infect others.
Three days after the World Health Organisation issued its revised advice on wearing masks, Dr. Maria Van Kerkhove, Head of the World Health Organisation’s emerging diseases and zoonosis unit, at a news briefing from the United Nations agency’s Geneva headquarters, reported that:
‘From the data we have, it still seems to be rare that an asymptomatic person actually transmits onward to a secondary individual. We have a number of reports from countries who are doing very detailed contact tracing. They’re following asymptomatic cases. They’re following contacts. And they’re not finding secondary transmission onward. It’s very rare.’
This is not what the UK Government or other governments around the world wanted to hear in order to justify keeping their populations under lockdown and imposing measures such as wearing masks, and the very next day Dr. Kerkhove was forced to retract her statements, and articles that had reported her remarks were rewritten in another of the increasing examples of censorship of online information that contradicts government policy. Now, according to Dr. Kerkhove’s revised statement, the rarity of asymptomatic transmission of the coronavirus only applies to a ‘small subset of studies’, as if all scientific research didn’t extrapolate from the particular to the general. Not only that, but now other modelling studies apparently estimate that ‘up to 40 per cent of coronavirus infections’ could be transmitted by asymptomatic persons. Not content with this global retraction worthy of the Moscow Show Trials or the House Un-American Activities Committee, Facebook has marked any article carrying Dr. Kerkhove’s remarks posted on its platform as ‘false information’ following a supposedly independent ‘fact check’.
From a scientific perspective, Dr. Kerkhove’s sudden change of medical opinion is difficult to explain; but from a political perspective it is easy. As explicable as the revision upwards of figures from the report on ‘Estimating infection prevalence in Wuhan City from repatriation flights’ published by Imperial College London on 9 March (in which the Infection Fatality Rate of coronavirus was estimated at 4.3 per cent, and the proportion of people between 70 and 79 years of age requiring hospitalisation was estimated at 16.6 per cent), to the 16 March report by the same team on the ‘Impact of non-pharmaceutical interventions (NPIs) to reduce COVID-19 mortality and healthcare demand’ (in which the IFR had been raised to 5.1 per cent and the hospitalisation rate to 24.3), thereby producing the since discredited estimates of the number of deaths from COVID-19 necessary to justify the Government imposed lockdown of the UK. Or as explicable as the World Health Organisation revising its advice on mask wearing on the same day the UK Government made the wearing of masks mandatory on public transport. It isn’t surprising that the new estimate, quoted by the chastened Dr. Kerkhove, that 40 per cent of infections come from pre-symptomatic persons originates from a report published by Imperial College London on 23 April, and led by the discredited Professor Neil Ferguson, the Government’s go-to expert for prophecies of doom that have repeatedly been proven wrong by many orders of magnitude. It should be apparent to even the most naïve observer that the technical lead on the World Health Organisation’s response to the coronavirus crisis wouldn’t change her mind overnight just because, as the media has reported, epidemiologists around the world complained. She changed it because it didn’t fit with what the governments of the world are telling their populations. In other words, this is another example of political expediency, rather than scientific opinion, dictating social policy.
But, fortunately, we don’t have to rely on Dr. Kherkove’s conscience in order to question the unquestioned orthodoxy of the claim that asymptomatic people can spread the virus. On 13 May, the Elsevier Public Health Emergency Collection published a report in the US National Library of Medicine titled ‘A study on infectivity of asymptomatic SARS-CoV-2 carriers’. Written by Chinese doctors working in Guangdong Provincial People’s Hospital, this had been able to trace and test 455 individuals — 35 hospital patients, 196 family members and 224 hospital staff — who had been brought into contact with an asymptomatic patient admitted to hospital in January and subsequently found to be infected with SARs-CoV-2. They concluded:
‘It is debatable whether asymptomatic COVID-19 virus carriers are contagious. The median contact time for patients was four days and that for family members was five days. No severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infections was detected in 455 contacts by nucleic acid test.
‘In summary, all the 455 contacts were excluded from SARS-CoV-2 infection and we conclude that the infectivity of some asymptomatic SARS-CoV-2 carriers might be weak. This finding implies that there is no need to worry unduly for asymptomatic or mild patients during the ongoing COVID-19 pandemic.
‘Under the development of epidemic circumstance, more and more public concern is on the increasing number of asymptomatic or mild patients hid in the community. However, combined with our results and the defense measures currently completed, we hope such worries are misplaced.’
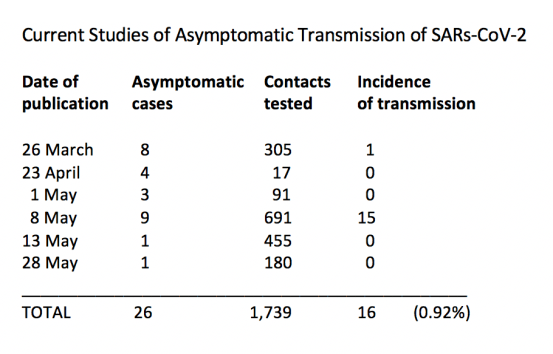
Another study on ‘Modes of contact and risk of transmission in COVID-19 among close contacts’, published on 26 March, tested 305 contacts of 8 asymptomatic cases and found 1 instance of secondary transmission. A study on ‘Coronavirus Disease Outbreak in Call Center, South Korea’, published on 23 April, found 4 asymptomatic cases out of 97 infections, and, again, none of their 17 household contacts acquired secondary infections. A study on ‘Contact Tracing Assessment of COVID-19 Transmission Dynamics in Taiwan and Risk at Different Exposure Periods Before and After Symptom Onset’, published on 1 May, reported that ‘none of the 9 asymptomatic case patients transmitted a secondary case’ to their 91 close contacts. A study on ‘SARS-CoV-2 transmission in different settings: Analysis of cases and close contacts from the Tablighi cluster in Brunei Darussalam’, published on 8 May, reported that among 9 cases with 691 contacts there were 15 incidence of secondary transmission. A summary review of medical studies ‘Estimating the extent of asymptomatic COVID-19 and its potential for community transmission: systematic review and meta-analysis’, published on 10 May, found that, among these four studies providing direct evidence of asymptomatic transmission, the rate of infection among 1,091 study cases ranged from none to 2.2 per cent. And a study reporting ‘No evidence of secondary transmission of COVID-19 from children attending school in Ireland, 2020’, published on 28 May, found that an asymptomatic schoolchild with SARs-CoV-2 who came into close or casual contact with 180 people resulted in ‘no confirmed cases of COVID-19’. It’s been established that asymptomatic persons can transmit SARs-CoV-2, but these figures (summarised in the table below) do not support the irresponsible and fearmongering claim that everybody is a potential threat of infection to everybody else.
The UK Government’s intention to enforce the wearing of masks on public transport is not only without legality, therefore, but it also has no proven basis in medical science. It is, rather — as the World Health Organisation’s revised advice on 5 June suggests — a means of enforcing further compliance with lockdown measures that have already condemned this country to what the Bank of England has predicted will be the worst depression in over 300 years, pushed unemployment to exceed an estimated 3 million, bankrupted thousands of small businesses, and caused the death of thousands of British citizens through the unnecessary and irresponsible cancellation of life-saving medical treatment, all while the Government sells our personal medical data to US tech firms, outsources our National Health Service to private companies, and in the absence of parliamentary scrutiny or approval makes legislation and regulations in violation of our human rights and civil liberties.
Addendum. On 20 November, a study published in Nature, one of the world’s leading multidisciplinary science journals, titled ‘Post-lockdown SARS-CoV-2 nucleic acid screening in nearly ten million residents of Wuhan, China’ reported that, out of 9,899,828 residents and 92.9 per cent of the population of Wuhan tested between 14 May and 1 June a month after lockdown restrictions were lifted on 9 April, no new symptomatic cases and just 300 asymptomatic cases were identified. From the latter, no positive tests for SARS-CoV-2 were identified among 1,174 close contacts of asymptomatic cases. Further testing of 52,312 samples between 13 June 13 and 2 July found no positive results; and two months after the screening of nearly 10 million residents, by 9 August there were still no newly confirmed cases of COVID-19 in the city most severely affected by COVID-19 in China. Statistically speaking, as a vector of infection, the asymptomatic transmission of SARS-CoV-2 doesn’t exist.
4. Surveillance and Compliance
There are other countries in which the wearing of masks has become customary, if not yet mandatory. Japan has a long history of wearing masks, going back to the so-called Spanish flu of 1919, the global flu epidemic of 1934, and the rise in pollution levels in the 1950s during rapid industrialisation. However, following the outbreak of SARs (severe acute respoiratory syndrome) in 2002, the panic around avian influenza in 2006, and the Ebola epidemic in 2014, wearing masks in public has become an increasingly-expected and enacted civic duty in China, Hong Kong, Japan, South Korea and Taiwan, and the recent influx of East-Asians into London in particular has brought the practice to the UK. We should recall that since 2002 SARs has killed a reported 774 people worldwide, bird flu 616, and Ebola over 11,000 people, almost entirely in West Africa; so the uniform wearing of masks in public among the 1.677 billion population of East Asia is out of all proportion to the actual threat of infection.
We would be wrong, however, to see the wearing of masks as only a matter of convention that should be uncritically imported into the UK as part of our response to the coronavirus crisis. In many East Asian countries the wearing of masks in certain public places such as hospitals and schools was made mandatory by their governments long before the coronavirus crisis, and Western observers have not been blind to their role in normalising and encouraging compliance with other measures of population surveillance and control. On 6 April, in an article titled ‘Coronavirus and the Future of Surveillance’ published first in Foreign Affairs (a forum for discussion of US foreign policy) and then in Belt & Road News (an organ of China’s global strategy for infrastructure development and investments in nearly 70 countries and international organisations), Nicholas Wright, a medical doctor and neuroscientist who works on emerging technologies and global strategy at University College London, the New America think-tank and the Georgetown University Medical Center, argued that one of the significant ‘legacies’ of the coronavirus crisis will be the spread of digital surveillance enabled by artificial intelligence, and that Western liberal democracies must keep pace with East Asia.
Citing the ‘arsenal of surveillance tools’ available to the governments of China, Hong Kong, South Korea and Taiwan to track and monitor their populations — which include the mass surveillance of mobile phone, rail, and flight data; deploying hundreds of thousands of neighbourhood monitors to log the movements and temperatures of individuals; integrating health and other databases so that hospitals, clinics, and pharmacies can access the travel information of their patients; tracking down individuals suspected of being infected by looking at credit card transactions and CCTV footage; enforcing self-quarantine through a location-tracking smartphone app; requiring government-issued identity cards in order to buy SIM cards or tickets on state-run rail companies and airlines; employing colour-coded smartphone apps that tag people as green, and therefore free to travel through city checkpoints, or as orange or red, and subject to restrictions on movement; and using facial recognition algorithms to identify commuters who aren’t wearing a mask or who aren’t wearing one properly — Wright argued that:
‘Western democracies must rise to meet the need for “democratic surveillance” to protect their own populations. One of COVID-19’s most important long-term impacts will be the reshaping of digital surveillance across the globe, prompted by the public health need to more closely monitor citizens.
‘Just as the September 11 attacks ushered in new surveillance practices in the United States, the coronavirus pandemic might do the same for many nations around the world. Afflicted countries are all eager to better control their citizens. Every functioning state now has a public health strategy to tackle COVID-19 that emphasises both monitoring residents and trying to influence their behaviour.
‘Western liberal democracies must be unafraid in trying to sharpen their powers of surveillance for public health purposes. There is nothing oxymoronic about the idea of “democratic surveillance”.’
5. Civil Disobedience
Many of us strongly disagree. In opposition to this dystopian vision of a surveillance state envisaged, significantly, not by an agent of the UK’s security forces but by a member of the medical profession, I recall the recent words of the Italian philosopher of bio-politics, Giorgio Agamben, who in one of his commentaries on the Italian Government’s use of the coronavirus to implement a surveillance state under a permanent state of emergency, reminded us that:
‘A rule which states that good must be renounced in order to save the good is just as false and contradictory as that which, in order to protect freedom, orders us to renounce freedom.’
The decision of a UK citizen to comply with the Government’s attempt to enforce the wearing of masks in public is not a private decision, therefore, but a political one that affects all of us, and we must oppose it individually and collectively with mass demonstrations of non-compliance. I hope that UK citizens will unite in civil disobedience to this unjustified, disproportionate and unlawful violation of our human rights, and refuse either to wear a mask or to pay the fixed penalty notice for not doing so.
The UK Government has announced that it is in the process of rolling out a joint private-public system of biosecurity that will extend the existing emergency period for years, and most likely for the rest of our lives. We have a very small window of opportunity to stop this while there is still some doubt and anger in the public’s mind about what the Government has done to the country, and the programme to test and trace us is still in development. As I have written elsewhere, once it’s up and running, the very notion of human rights will effectively be over. Either we do what the Government tells us, or our individual access to public life, spaces and services will be removed. The mandatory wearing of masks on public transport is a test of our compliance to such forms of control; but over the past four months the UK Government has been repeatedly testing the British public for how much loss of liberty we will accept — whether it’s house arrest, enforced social distancing, sharing our medical data with private corporations, moving further education online, digitally tracking our movements and contacts, requiring biometric immunity passports to access public spaces, or imposing curfews — and at every test we have failed. This passive acquiescence and total lack of resistance must stop now.
If enough of us take a stand against this further unnecessary encroachment on our civil liberties, we can look forward to thousands of court cases in which the Crown Prosecution Service will have to prove the scientific validity of wearing masks to combat a virus that has been circulating in the UK for at least 5 months now. To this end, I hope both human rights lawyers (with Doughty Street Chambers having already published advice on challenging the thousands of unlawful arrests, prosecutions and fines issued by the police for not obeying Government guidelines) and medical practitioners will step forward to support us in challenging the Government’s right to enforce a permanent programme of bio-security on the UK population under the guise of protecting us from COVID-19. If we don’t, this will not be the last so-called emergency measure imposed on the British public under the cloak of the coronavirus crisis. Now more than ever, we must stand up to the propaganda and lies of this Government.
Appendix: Medical Advice against Wearing Masks
Below is a chronologically arranged (with the most recent first) compendium of medical opinion and advice against the use of masks, both medical and hand-made, by members of the public in non-healthcare settings. These opinions include not only the repeated statements to this effect by the World Health Organisation but also those of the UK Government’s own Scientific Advisory Group on Emergencies (SAGE) and the Deputy Chief Medical Officer for England. There is, admittedly, medical opinion in favour of using masks, much of it made following the announcement of the Government guidance making it mandatory, but these already have widespread dissemination in our national press and media. The purpose of this compendium is to arm those who have decided to ignore these guidelines with medical opinions and arguments in support of their civil disobedience.
‘The recommendation to wear surgical masks to supplement other public health measures did not reduce the SARS-CoV-2 infection rate among wearers by more than 50% in a community with modest infection rates, some degree of social distancing, and uncommon general mask use. The data were compatible with lesser degrees of self-protection.’
— Annals of Internal Medicine, 18 November, 2020*
(Unlike the usual observational study of mask wearers, this is the first randomised controlled trial, making it the highest quality scientific evidence to date. However, although the study was conducted in April and May, the results of its findings meant its publication was delayed, with the study refused by three medical journals, the Lancet, the New England Journal of Medicine and the Journal of the American Medical Association.)
‘ACP [American College of Physicians] discourages the use of N95 respirators by asymptomatic or symptomatic persons in community settings to reduce the risk for SARs-CoV-2 infection in the absence of any demonstrated benefit.
‘Potential harms associated with mask use include self-contamination, breathing difficulties, and a false sense of security that could potentially detract from taking other precautions, such as physical distancing.
‘The goal of using N95 respirators, surgical masks, or cloth masks is to prevent transmission of SARS-CoV-2 infection from asymptomatic or symptomatic infected persons to uninfected persons (source control). Currently, no direct evidence exists for the effectiveness or comparative effectiveness of various types of respirators or masks for preventing SARS-CoV-2 infection in community settings.
‘N95 respirators should not be used in a community setting, given the absence of demonstrated benefit, the possible harm with improper use (that is, the requirement for fit testing), and the global shortage of N95 respirators.’
— 18 June, 2020
Advice on the use of masks in the context of COVID-19
‘At the present time, the widespread use of masks by healthy people in the community setting is not yet supported by high quality or direct scientific evidence and there are potential benefits and harms to consider (see below).
Potential benefits/advantages
‘The likely advantages of the use of masks by healthy people in the general public include:
- reduced potential exposure risk from infected persons before they develop symptoms;
- reduced potential stigmatization of individuals wearing masks to prevent infecting others (source control) or of people caring for COVID-19 patients in non-clinical settings;
- making people feel they can play a role in contributing to stopping spread of the virus;
- reminding people to be compliant with other measures;
- potential social and economic benefits. Amidst the global shortage of surgical masks and PPE, encouraging the public to create their own fabric masks may promote individual enterprise and community integration. Moreover, the production of non-medical masks may offer a source of income for those able to manufacture masks within their communities. Fabric masks can also be a form of cultural expression, encouraging public acceptance of protection measures in general. The safe re-use of fabric masks will also reduce costs and waste and contribute to sustainability.’
Potential harms/disadvantages
‘The likely disadvantages of the use of mask by healthy people in the general public include:
- potential increased risk of self-contamination due to the manipulation of a face mask and subsequently touching eyes with contaminated hands;
- potential self-contamination that can occur if non- medical masks are not changed when wet or soiled. This can create favourable conditions for microorganism to amplify;
- potential headache and/or breathing difficulties, depending on type of mask used;
- potential development of facial skin lesions, irritant dermatitis or worsening acne, when used frequently for long hours;
- difficulty with communicating clearly;
- potential discomfort;
- a false sense of security, leading to potentially lower adherence to other critical preventive measures such as physical distancing and hand hygiene;
- poor compliance with mask wearing, in particular by young children;
- waste management issues; improper mask disposal leading to increased litter in public places, risk of contamination to street cleaners and environment hazard;
- difficulty communicating for deaf persons who rely on lip reading;
- disadvantages for or difficulty wearing them, especially for children, developmentally challenged persons, those with mental illness, elderly persons with cognitive impairment, those with asthma or chronic respiratory or breathing problems, those who have had facial trauma or recent oral maxillofacial surgery, and those living in hot and humid environments.’
— World Health Organisation (5 June, 2020).*
(*On 12 July, Deborah Cohen, the Health Correspondent for BBC Newsnight, former investigations editor for the British Medical Journal for 13 years, with a Bachelor of Medicine and Bachelor of Surgery degrees from the University of Manchester, in a programme on the debate around the use of masks broadcast the previous Friday, 10 June, reported (6’06”): ‘The debate is deeply political. Newsnight understands that the World Health Organisation committee that reviewed the evidence for the use of face coverings in public didn’t back them. But after political lobbying, the WHO now recommends them.’ This attracted outrage and attacks among mask-promoters on Twitter, leading Ms. Cohen to confirm on her personal page: ‘We had been told by various sources [the] WHO committee reviewing the evidence had not backed masks but they recommended them due to political lobbying. This point was put to WHO who did not deny [it].’)
Expert reaction to mandatory face masks on public transport
‘The World Health Organisation’s advice is clear. Although a medical mask can offer some protection, the use of masks in a community setting is not supported. Furthermore, mask wearing can result in a false sense of security, and enhanced risks that come from touching the face. This seems to me to be another political decision, rather than one based on scientific evidence.’
— Professor Nicola Stonehouse, Professor of Molecular Virology, University of Leeds (4 June, 2020)
‘The issue of face coverings in the context of the COVID-19 pandemic is very controversial. While no ad-hoc studies with a correct design have been carried out, it is now commonly accepted that face coverings provide very little protection, if any. However, there are many potential side effects of face coverings from a clinical and epidemiological point of view, although none of them has been studied.
- ‘Will more people use the tube/buses because they will feel more secure given that everybody wears a face covering? This will increase the risk of transmission.
- ‘Will people be able not to contaminate their hands and the handrails by not touching their face coverings and not touching the handrails while standing inside buses and trains? This seems to be impossible to me. Face coverings can therefore be a vehicle of infection, rather than a barrier.’
— Dr. Antonio Lazzarino, Department of Epidemiology and Public Health, University College London
‘This policy will add more burden on the general public to prevent the spread of COVID-19. This is much more complicated than “wash your hands for 20 seconds” or “stay at home”. We are asking the whole population of Britain, with no prior experience of mask-wearing, to overnight become competent makers, wearers, and maintainers of PPE. I hope the Government has a fool-proof plan in place to educate every family in the country on how to do this, or it could actually put people at higher risk of infection.
‘Wearing a basic face mask does little or very little to prevent the wearer from getting infected by others, but there is some limited evidence that wearing one can prevent others from being infected by the wearer. I have seen no new evidence to suggest why the Government is reversing its previous policy, and ignoring its previous scientific guidance and the guidance of the WHO. I’m left wondering if this is a political decision, rather than one based on science.
‘If this change in policy is to be successful at reducing infections, it will have to be accompanied by a major new campaign to educate 66 million people on how to properly make, put on, handle and clean their face coverings. A badly-fitted, damp or dirty mask, or poor habits such as regularly touching eyes or adjusting the ties, can put the wearer at greater risk of infection.’
— Dr Simon Clarke, Associate Professor in Cellular Microbiology, University of Reading (4 June, 2020)
‘Disposable medical masks (also known as surgical masks) are loose-fitting devices that were designed to be worn by medical personnel to protect accidental contamination of patient wounds, and to protect the wearer against splashes or sprays of bodily fluids. There is limited evidence for their effectiveness in preventing influenza virus transmission either when worn by the infected person for source control or when worn by uninfected persons to reduce exposure. Our systematic review found no significant effect of face masks on transmission of laboratory-confirmed influenza.
‘We did not consider the use of respirators in the community. Respirators are tight-fitting masks that can protect the wearer from fine particles and should provide better protection against influenza virus exposures when properly worn because of higher filtration efficiency. However, respirators work best when they are fit-tested, and these masks will be in limited supply during the next pandemic. These specialist devices should be reserved for use in healthcare settings or in special subpopulations such as immunocompromised persons in the community, first responders, and those performing other critical community functions, as supplies permit.
‘In lower-income settings, it is more likely that reusable cloth masks will be used rather than disposable medical masks because of cost and availability. There are still few uncertainties in the practice of face mask use, such as who should wear the mask and how long it should be used for. In theory, transmission should be reduced the most if both infected members and other contacts wear masks, but compliance in uninfected close contacts could be a problem. Proper use of face masks is essential because improper use might increase the risk for transmission.’
— Centers for Disease Control and Infection (May 2020)
Universal Masking in Hospitals in the Covid-19 Era
‘We know that wearing a mask outside health care facilities offers little, if any, protection from infection. Public health authorities define a significant exposure to Covid-19 as face-to-face contact within 6 feet with a patient with symptomatic Covid-19 that is sustained for at least a few minutes (and some say more than 10 minutes or even 30 minutes). The chance of catching Covid-19 from a passing interaction in a public space is therefore minimal. In many cases, the desire for widespread masking is a reflexive reaction to anxiety over the pandemic.’
— New England Journal of Medicine (21 May, 2020)
Impact of non-pharmaceutical interventions against COVID-19 in Europe: a quasi-experimental study
‘The use of face coverings initially seems to have had a protective effect. However, after day 15 of the face covering advisories or requirements, the number of cases started to rise. Similar patterns were observed for the relationship between face coverings and deaths. Negative associations were estimated for mass gatherings, initial business closure and the closure of educational facilities; while a non-significant effect was estimated for non-essential business closure. There was a positive association with the usage of face coverings (masks), while the stay-home measures showed an inverted U quadratic effect with an initial rise of cases up to day 20 of the intervention followed by a decrease in cases. These results would suggest that the widespread use of face masks or coverings in the community do not provide any benefit. Indeed, there is even a suggestion that they may actually increase risk, but as stated previously, we feel that the data on face coverings are too preliminary to inform public policy.’
— Professor Paul Raymond Hunter, Norwich Medical School, University of East Anglia; Dr. Julii Suzanne Brainard, University of East Anglia; Dr. Felipe Colon-Gonzalez, London School of Hygiene and Tropical Medicine; Dr. Steve Rushton, University of Newcastle (6 May, 2020)
‘The evidence on effectiveness of mask for source control (i.e. stopping infectious people — pre-symptomatic/asymptomatic — from infecting others) is weak. Evidence for protecting the mask wearer from becoming infected is also weak.
‘The effect of wearing a mask is likely to be small but not zero. The RCT [randomised clinical trial] evidence is weak and it would be unreasonable to claim a large benefit from wearing a mask.
‘SAGE advice below refers to cloth masks — specifically in the context of lockdown measures.
‘Negative behavioural impacts cannot be ruled out, e.g. those with symptoms who should isolate instead choose to break quarantine wearing a mask, or repeated handling of mask could increase hand-face contact.
‘Wearing masks in the context of lifting NPIs [non-pharmaceutucal interventions] could reduce anxiety about release of emasures, or reinforce the need for distancing measures.’
— Minutes of the 27th meeting of the Scientific Advisory Group on Emergencies (21 April, 2020)
Do face masks work? A note on the evidence
‘When a person is infectious with a virus it is estimated that they may shed one hundred billion virus particles a day — that works out at about ten million per breath. A mask won’t stop you putting these particles into the air around you. In fact, with a damp mask you’ll be blowing aerosols and larger particles sideways, directly at your socially distanced colleagues two metres away. And if wearing a mask tempts you to feel that you’re not going to infect anyone else, you may also be less likely to observe the two-metre rule. So does wearing a mask protect others if you’re infectious? There’s little direct evidence to say that it does, and quite a lot of straightforward reasoning to suggest it doesn’t.’
‘The point is: does any of what is out there add up to a watertight case for compelling people to wear masks in public or at work (outside a healthcare setting)? The threshold for compulsion must surely be higher than ‘maybe’ and ‘perhaps’. But if it really is the case that the threshold for regulatory compulsion is being approached, it should be a simple matter for our scientific advisors to present it to us and allow time for it to be critically discussed in relation to a real-world setting, before Government imposes measures upon us all. That other countries may have taken action says things about those countries’ attitudes to open scrutiny of evidence-based decision-making, and their populations’ attitudes to compliance and compulsion. It says nothing about the validity of the measures.’
— Dr. John Lee, former professor of pathology and NHS consultant pathologist (19 April, 2020)
Masks Don’t Work: A review of science relevant to Covid-19 social policy
‘Masks and respirators do not work. There have been extensive randomized controlled trial (RCT) studies, and meta-analysis reviews of RCT studies, which all show that masks and respirators do not work to prevent respiratory influenza-like illnesses, or respiratory illnesses believed to be transmitted by droplets and aerosol particles.
‘Furthermore, the relevant known physics and biology, which I review, are such that masks and respirators should not work. It would be a paradox if masks and respirators worked, given what we know about viral respiratory diseases: The main transmission path is long-residence-time aerosol particles (<2.5μm), which are too fine to be blocked, and the minimum-infective-dose is smaller than one aerosol particle.
‘The present paper about masks illustrates the degree to which governments, the mainstream media, and institutional propagandists can decide to operate in a science vacuum, or select only incomplete science that serves their interests. Such recklessness is also certainly the case with the current global lockdown of over 1 billion people, an unprecedented experiment in medical and political history.’
— D. G. Rancourt, Ontario Civil Liberties Association, former tenured and Full Professor of physics at the University of Ottawa, Canada (11 April, 2020)
Advice on the use of masks in the context of COVID-19
‘There is limited evidence that wearing a medical mask by healthy individuals in the households or among contacts of a sick patient, or among attendees of mass gatherings may be beneficial as a preventive measure. However, there is currently no evidence that wearing a mask (whether medical or other types) by healthy persons in the wider community setting, including universal community masking, can prevent them from infection with respiratory viruses, including COVID-19.
‘The wide use of masks by healthy people in the community setting is not supported by current evidence and carries uncertainties and critical risks. WHO stresses that it is critical that medical masks and respirators be prioritized for health care workers. The use of masks made of other materials (e.g., cotton fabric), also known as nonmedical masks, in the community setting has not been well evaluated. There is no current evidence to make a recommendation for or against their use in this setting.’
— World Health Organisation (6 April 2020)
‘Neither surgical nor cotton masks effectively filtered SARS–CoV-2 during coughs by infected patients. Prior evidence that surgical masks effectively filtered influenza virus informed recommendations that patients with confirmed or suspected COVID-19 should wear face masks to prevent transmission. However, the size and concentrations of SARS–CoV-2 in aerosols generated during coughing are unknown. Oberg and Brousseau demonstrated that surgical masks did not exhibit adequate filter performance against aerosols measuring 0.9, 2.0, and 3.1 μm in diameter. Lee and colleagues showed that particles 0.04 to 0.2 μm can penetrate surgical masks. The size of the SARS–CoV particle from the 2002–2004 outbreak was estimated as 0.08 to 0.14 μm; assuming that SARS-CoV-2 has a similar size, surgical masks are unlikely to effectively filter this virus.
‘This experiment did not include N95 masks and does not reflect the actual transmission of infection from patients with COVID-19 wearing different types of masks. We do not know whether masks shorten the travel distance of droplets during coughing. Further study is needed to recommend whether face masks decrease transmission of virus from asymptomatic individuals or those with suspected COVID-19 who are not coughing.
‘In conclusion, both surgical and cotton masks seem to be ineffective in preventing the dissemination of SARS–CoV-2 from the coughs of patients with COVID-19 to the environment and external mask surface.’
— Annals of Internal Medicine (6 April, 2020). This article was subsequently withdrawn at the request of the editors.
Masks-for-all for COVID-19 not based on sound data
‘We do not recommend requiring the general public who do not have symptoms of COVID-19-like illness to routinely wear cloth or surgical masks because:
- There is no scientific evidence they are effective in reducing the risk of SARS-CoV-2 transmission;
- Their use may result in those wearing the masks to relax other distancing efforts because they have a sense of protection;
- We need to preserve the supply of surgical masks for at-risk healthcare workers.
‘Sweeping mask recommendations — as many have proposed — will not reduce SARS-CoV-2 transmission, as evidenced by the widespread practice of wearing such masks in Hubei province, China, before and during its mass COVID-19 transmission experience earlier this year. Our review of relevant studies indicates that cloth masks will be ineffective at preventing SARS-CoV-2 transmission, whether worn as source control or as PPE.
‘We realize that the public yearns to help protect medical professionals by contributing homemade masks, but there are better ways to help.
‘Given the paucity of information about their performance as source control in real-world settings, along with the extremely low efficiency of cloth masks as filters and their poor fit, there is no evidence to support their use by the public or healthcare workers to control the emission of particles from the wearer.
‘Leaving aside the fact that they are ineffective, telling the public to wear cloth or surgical masks could be interpreted by some to mean that people are safe to stop isolating at home. It’s too late now for anything but stopping as much person-to-person interaction as possible.
‘Masks may confuse that message and give people a false sense of security. If masks had been the solution in Asia, shouldn’t they have stopped the pandemic before it spread elsewhere?
‘For readers who are disappointed in our recommendations to stop making cloth masks for themselves or healthcare workers, we recommend instead pitching in to locate N95 FFRs and other types of respirators for healthcare organizations. Encourage your local or state government to organize and reach out to industries to locate respirators not currently being used in the non-healthcare sector and coordinate donation efforts to frontline health workers.’
— Centre for Disease Research and Policy (1 April, 2020)
COVID-19, shortages of masks and the use of cloth masks as a last resort
Critical shortages of personal protective equipment (PPE) have resulted in the US Centers for Disease Control downgrading their recommendations for health workers treating COVID-19 patients from respirators to surgical masks and finally to home-made cloth masks. As authors of the only published randomised controlled clinical trial of cloth masks, we have been getting daily emails about this from health workers concerned about using cloth masks. The study found that cloth mask wearers had higher rates of infection than even the standard practice control group of health workers, and the filtration provided by cloth masks was poor compared to surgical masks.
— British Medical Journal (30 March, 2020)
Face masks could increase risk of infection
‘For the average member of the public wandering down a street this is really not a good idea. What tends to happen is people will have one mask. They won’t wear it all the time. They will take it off when they get home. They’ll put it down on a surface they haven’t cleaned. Or they will be out — they haven’t washed their hands — and they’ll go and have a cup of coffee somewhere. They half hook it off, they wipe something over it, they’ll put it back on. And, in fact, you can actually trap the virus in the mask and start breathing it in. Because of these behavioural issues, which are really important when talking about infectious diseases, people can adversely put themselves at more risk than less.’
— Dr. Jenny Harries, Deputy Chief Medical Officer for England (12 May, 2020)
‘There is a moderate overall quality of evidence that face masks do not have a substantial effect on transmission of influenza.
‘Face mask use is common to prevent transmission of infections in health care settings around the world, and a widely used measure in some communities, particularly in South-East Asia.
‘Reusable cloth face masks are not recommended. Medical face masks are generally not reusable, and an adequate supply would be essential if the use of face masks was recommended. If worn by a symptomatic case, that person might require multiple masks per day for multiple days of illness.’
— World Health Organisation (October 2019)
Why face masks don’t work: A revealing review
‘The science regarding the aerosol transmission of infectious diseases has, for years, been based on what is now appreciated to be “very outmoded research and an overly simplistic interpretation of the data”. Modern studies are employing sensitive instruments and interpretative techniques to better understand the size and distribution of potentially infectious aerosol particles.
‘It should be concluded from these and similar studies that the filter material of face masks does not retain or filter out viruses or other submicron particles. When this understanding is combined with the poor fit of masks, it is readily appreciated that neither the filter performance nor the facial fit characteristics of face masks qualify them as being devices which protect against respiratory infections.
‘Between 2004 and 2016 at least a dozen research or review articles have been published on the inadequacies of face masks. All agree that the poor facial fit and limited filtration characteristics of face masks make them unable to prevent the wearer inhaling airborne particles. In their well-referenced 2011 article on respiratory protection for healthcare workers, Drs. Harriman and Brosseau conclude that “facemasks will not protect against the inhalation of aerosols.”
‘The primary reason for mandating the wearing of face masks is to protect dental personnel from airborne pathogens. This review has established that face masks are incapable of providing such a level of protection. Unless the Centers for Disease Control and Prevention, national and provincial dental associations and regulatory agencies publically admit this fact, they will be guilty of perpetuating a myth which will be a disservice to the dental profession and its patients.’
— John Hardie, BDS, MSc, PhD, FRCDC, Oral Health (18 October, 2016). Like so much published online that contradicts Government policy, this article has since been removed from its original location on the internet, but it can still be accessed here: Why face masks don’t work.
A cluster-randomised trial of cloth masks compared with medical masks in healthcare workers
‘This study is the first RCT [randomised clinical trial] of cloth masks, and the results caution against the use of cloth masks. This is an important finding to inform occupational health and safety. Moisture retention, reuse of cloth masks and poor filtration may result in increased risk of infection. Further research is needed to inform the widespread use of cloth masks globally.’
— British Medical Journal (2015)
If you know of additional medical advice against the wearing of hand-made masks by the public, please copy a link in the comments section below and I will add it to this compendium.
Addendum 1. New Regulations on Wearing Masks on Public Transport
As the Government indicated to the public on 12 June, a mere 3 days before it came into force, a statutory instrument was today made into law under the emergency procedure set out in Section 45R of the Public Health (Control of Disease) Act 1984. This is the latest of the 102 coronavirus-related statutory instruments laid before Parliament; and in accordance with this legislation on ‘emergency procedure’, the Health Protection (Coronavirus, Wearing of Face Coverings on Public Transport) (England) Regulations 2020 were made without a draft having been laid before and approved by a resolution of each House of Parliament. The reason given for this circumvention of the legislature, as it was for the Health Protection (Coronavirus, Restrictions) (England) Regulations 2020 (the Regulations) that came into force on 26 March, is as follows:
‘It is the opinion of the Secretary of State that, by reason of urgency, it is necessary to make the order without a draft being so laid and approved so that public health measures can be taken in response to the serious and imminent threat to public health which is posed by the incidence and spread of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).’
It is unclear how, 3 months after social distancing guidelines were issued by the Government on 16 March and the subsequent lockdown of the UK was imposed on 23 March, there can be sufficient urgency and insufficient time to justify circumventing scrutiny and approval by our elected representatives in Parliament of Regulations on a policy that has been considered by the Government for months and will now be imposed by UK police forces on tens of millions of British citizens. Just as it is unclear how the present situation constitutes a ‘serious and imminent threat to public health’ when, between 25 May and 7 June, the National Office for Statistics estimated just 0.06 per cent of the population in England, or 1 in 1,700 people, were infected with SARs-CoV-2; when, by 9 June, the NHS reported that only 294 people under the age of 60 without pre-existing medical conditions had died in English hospitals with their deaths attributed to COVID-19; when, the day before these Regulations were published, the Government itself attributed just 36 deaths to COVID-19; and the Government’s own estimated rate of reproduction for every person infected in the UK is between 0.2 and 0.7. But without providing evidence of either their justification or proportionality, these Regulations:
- Come into force on 15th June 2020, and apply to English land, sea and airspace.
- Defines a ‘face covering’ as anything that covers a person’s nose and mouth, the mandatory wearing of which applies on public transport, excluding school transport, taxis or private hire and cruise ships.
- Prohibits any person, without ‘reasonable excuse’, from using public transport without wearing a face covering. This does not include any child under 11 years of age; any employee of the operator of the relevant public transport service in the course of their employment; a constable or police community support officer acting in the course of their duty; an emergency responder; a relevant official; or anyone in an enclosed cabin, berth or car on a ship who is alone or with members of the same household.
- Defines a reasonable excuse as any physical or mental illness or impairment, or disability; or severe distress caused by wearing a face covering; or travelling with someone who relies on lip reading to communicate; or to avoid harm or injury; or in order to eat or drink; or to take medication; or upon direction by a ‘relevant person’.
- Defines a relevant person as a police constable; a police community support officer; or a public transport officer, employee or agent authorised by the operator for the purposes of this regulation. This Regulation empowers such persons to deny boarding of a vehicle providing a public transport service to a person not wearing a face covering; to direct a person either to wear a face covering or to disembark from a relevant vehicle. It additionally empowers a constable to remove a passenger from a relevant vehicle, using reasonable force if necessary, if they fail to comply with a direction to disembark from the vehicle. Imprtantly, the ‘Explanatory Memorandum’ to the Regulations adds that operators of public transport services ‘have discretion over whether they choose to use these powers; they do not have an obligation to do so’.
- Provides that any person who contravenes this regulation commits an offence, which is punishable by a fine.
- Empowers a fixed penalty notice, which enables a person to discharge their liability to criminal conviction, to be issued by a constable, police community support officer, a Transport for London officer, or any person designated by the Secretary of State for the purposes of this regulation, such as an operator of a public transport service. The fixed penalty notice can be issued to a person over 18 years of age whom such a person reasonably believes to have committed an offence under these Regulations. The amount of the fixed penalty is £100, reduced to £50 if paid within 14 days of a notice being issued.
- Empowers the Crown Prosecution Service and any person designated by the Secretary of State to bring proceedings for an offence under these Regulations.
- Requires the Secretary of State to review the need for the requirements imposed by the Regulations before the end of the period of 6 months, beginning with the day on which they come into force.
- Provides that these Regulations cease to have effect at the end of the period of 12 months, beginning with the day on which they come into force.
Despite an assessment of their impact not having been made, the Secretary of State for Transport has nonetheless said that, in his view, these Regulations are ‘compatible’ with the European Convention on Human Rights.
- He does not explain why, however, the general public are considered potential transmitters of SARs-CoV-2 of a sufficient degree of virulence to require the compulsory wearing of masks on public transport, and yet the constables, community support officers and transport staff tasked with policing the public every day, and therefore the most obvious source of viral contagion, are not.
- Nor does he explain why, given the £100 fixed penalty notice for diosobedience, a wealthier person should be more financially able to ignore these Regulations compared to a poorer person, implying that such a person represents less of a threat to public health.
- Nor does he explain whether a person must prove their ‘severe distress caused by wearing a face covering’ to a constable, community support officer or other relevant person, and if so how.
- Nor does he accept any legal responsibility, or indicate any commitment to financial compensation, for loss of life, or work or employment for anyone who — as is suggested by the numerous medical opinions quoted above — contracts SARs-CoV-2 or some other respiratory disease, or is exposed to any other medical complications, caused by breathing though and into the type of home-made masks they are compelled by these Regulations to wear on a daily basis and for extended periods of time in the enclosed and often humid environments that characterise public transport in the UK and particularly in London during the summer.
As serious, perhaps, as this cavalier and arbitrarily imposed approach to the health and safety of passengers on UK public transport is the fact that these Regulations have only been published on the day on which they come into effect, without assessment, scrutiny, debate or approval, thereby ignoring the division of powers — executive, legislature and judiciary — on which we rely for the democratic accountability of government. This has characterised and defined the huge number and reach of powers made by the Government under the cloak of the coronavirus crisis, and its latest use to impose politically motivated and medically unsubstantiated and even dangerous regulations indicates how the Government will roll out the even greater violations of our human rights and civil liberties by future programmes such as contact tracing, immunity passports and vaccination, which truly do present a ‘serious and imminent threat’ to the UK public.
Just five days ago, on 10 June, at the Fourth Delegated Legislation Committee to discuss the second amendment to the Health Protection (Coronavirus, Restrictions) (England) (Amendment) (No. 2) Regulations 2020, Justin Madders, the Member of Parliament for Ellesmere Port and Neston, questioned the Minister for Care, Helen Whately, about the procedure for considering these regulations. Pointing out that these were signed into law several weeks before, he made the following criticisms, which I will quote at length, not least because this is one of the very few examples of which I am aware of our elected representatives in Parliament attempting to hold the Government to account over its repeated and ongoing circumvention of parliament scrutiny of coronavirus legislation:
‘The Minister has said that it is right that the rule of law be maintained, and of course we agree with that, but I fear that, by debating these regulations retrospectively, we are treading on the wrong side of that. As I stated when we debated those initial regulations back on 4 May — some six weeks after they had been introduced — given that Parliament was up and running again by that time, there should have been sufficient time to ensure that future changes were debated and had democratic consent before they were introduced. Debating them weeks after the event, and when in fact they have already been superseded, as we have heard today, is frankly an insult.
‘There is no excuse for this situation now. As we have heard, the regulations require there to be a review every three weeks, as the Secretary of State has a duty to terminate any regulations that are not necessary or proportionate to control the transmission of the virus. That means that all along we have had a clear timetable and sight for when new regulations might be created, which should have allowed plenty of opportunity for parliamentary scrutiny of those regulations.
‘Yet here we are again today, debating regulations that came into effect weeks ago. That is not good enough. Moving forwards, we cannot carry on in this way and the Government accept our indolence at their peril. Does the Minister agree that debating regulations when they are already out of date makes a mockery of the process?
‘The Minister went on to say that the regulations are, in fact, constantly reviewed; I should be grateful if she would clarify exactly what she means by that. Is there a formal process by which that is taking place, or are there, in fact, just the three-weekly reviews that have been set out in the regulations?
‘As for those reviews, where are they? In a written question that I put to the Secretary of State for Health and Social Care, I asked if he would publish the reviews carried out on 16 April, 7 May and 28 May pursuant to these regulations. I received a reply to that question at half-past 9 last night, which said:
“The Department of Health and Social Care has indicated that it will not be possible to answer the question within the usual time period.”
‘I find that absolutely incredible, and, regrettably, the failure of the Department to provide me with an answer to what I would have thought was a pretty important and obvious question leads me to one inevitable and damning conclusion: there has been no proper review.
‘Here we have the most far-reaching impositions on the life of this country in peacetime, and the Government has not, as required by law, conducted any review of those regulations that we can actually see; or if they have, they have decided that we do not deserve to see them, which is equally reprehensible.
‘I understand, from what the Minister said in her introduction, that there were several more reviews on 22 April and 7 May. Again, if the Minister had not been good enough to tell us today about those reviews, we would never have known that they had taken place. We need far more transparency than we are seeing at the moment. We cannot go on like this.
‘It is because of their wide-ranging effect that these measures demand full parliamentary scrutiny. I am sure that many hon. Members agree that a 90-minute debate by a small parliamentary Committee, weeks after the fact, cannot possibly be sufficient to provide the level of examination and scrutiny that such important laws require. As we have seen, great efforts have been made by staff to get Parliament up and running again. We should not demean those efforts by turning these debates into a procedural formality, a rubber-stamping exercise to create the veneer of a democratic process. We should be better than that. We should not be debating the measures late and without the full extent of the information on which the Government have made their decisions.
‘When it comes to the regulations themselves, not only has the legally required review of them not been disclosed to date; they have not had any kind of impact assessment carried out. Again, to be fair to the Government, we understand why, in the first instance, that was not possible. However, we did make it very clear, the last time the regulations were debated, that we did not want that to become the norm, especially for regulations such as these, where we know that the impact will have been huge. The second and third set of regulations have apparently had no impact assessment, either. How can the Government continue to issue new laws with such sweeping powers as these when they cannot tell us what their impact is?’
As the latest instance of the ongoing making of the most draconian and intrusive laws in the history of the UK during peacetime, the unjustified and grossly disproportionate Health Protection (Coronavirus, Wearing of Face Coverings on Public Transport) (England) Regulations 2020 raise further questions for the legislature, judiciary and UK public about our ability to hold the executive to account under an ‘emergency period’ it is in the Government’s power to extend indefinitely. With public protests banned under the third amendment to the Health Protection (Coronavirus, Restrictions) (England) (Amendment) (No. 3) Regulations 2020 that came into force on 1 June and were approved by a virtual Parliament on 15 June; with the UK press and media embracing its role as an organ of Government propaganda devoted to spreading fear and silencing questions; with the Government free to make laws without parliamentary approval; with the UK judiciary silent and complicit in enacting these laws; with legislative procedures of review not being followed in any meaningful and accountable way; and with what scrutiny a virtual Parliament can attempt either ignored or dismissed by Ministers; we are, technically speaking — which is to say, in political terms — living under a legislative dictatorship.
Postscript. In the absence of either legislation or Government guidance on whether a person has to prove they have a ‘reasonable excuse’ for exemption from these Regulations — and if so how — in order to avoid a fixed penalty notice of £100 from a constable, community support office, Transport for London officer, employee or agent of a transport service operator, or any relevant person designated by the Secretary of State to impose these Regulations, I wrote to Transport for London — which has the discretion and not the obligation to use these powers — and in return was advised that on Friday, 19 June, TfL had introduced an ‘exemption card’ that customers of their services can either print out and carry or download onto their phone and produce on request, granting them exemption. The pdf for these cards is available on the TfL website page ‘Face coverings’. If challenged by a relevant person, and in the absence of any medical reason or duty of care, someone not wishing to travel on public transport with a covering over their face can state that, under Section 4, a), ii of the Health Protection (Coronavirus, Wearing of Face Coverings on Public Transport) (England) Regulations 2020, he or she is exempt because wearing such a covering causes them ‘severe distress’. If asked what the nature of this distress is, they might wish to direct the relevant person to the contents of this article.
Addendum 2. Further Regulations on Wearing Masks in Shops and Other Places
On 14 July, the Secretary for State for Health and Social Care announced to a House of Commons with less than two dozen MPs present that face coverings will become mandatory for customers in shops and supermarkets, with non-compliance punished with a fixed penalty notice up to £100:
‘Should an individual without an exemption refuse to wear a face covering, a shop can refuse them entry and can call the police if people refuse to comply. The police have formal enforcement powers and can issue a fine.
‘This is in line with how shops would normally manage their customers and enforcement is of course a last resort, and we fully expect the public to comply with the rules as they have done throughout the pandemic.’
In response to this announcement, the Chair of the Metropolitan Police Force told BBC Radio 4:
‘It will be nigh-on impossible for enforcement because you won’t have a police officer on every shop door because there isn’t enough of us. If a shopkeeper calls the police because someone hasn’t got a mask on, they haven’t got the power to detain them so that person can just walk away. We’ll be driving around and around London looking for people who aren’t wearing masks, it’s absolutely absurd.’
On 22 July, the Commissioner of the Metropolitan Police Force confirmed that her police officers will not respond to calls about shoppers refusing to wear face coverings, and that calling the police should be a ‘last resort’. She also told LBC Radio that she hoped shoppers would be ‘shamed’ into compliance:
‘My hope is that the vast majority of people will comply, and that people who are not complying will be shamed into complying or shamed to leave the store by the store keepers or by other members of the public.’
The following day, on 23 July, The Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) Regulations 2020 were finally published. Once again, these were made by Statutory Instrument under the Public Health (Control of Disease) Act 1984; once again without prior scrutiny by Parliament of the evidence; once again without an impact assessment having been made; and once again with the absence of all of these requirements justified ‘by reason of urgency’, despite the Regulations being made four months since the Government-imposed lockdown of the UK and as many since the debate on the benefits and dangers of wearing masks in public began.
Under Regulation 1, these Regulations come into force in England and Wales on 24 July, 2020. Under Regulation 3, we cannot enter or remain within a ‘relevant place’ without wearing a covering over our mouth and nose. Under Regulation 5, a ‘relevant person’ can deny us entry to, direct us to wear a face covering within, or direct us to leave, a ‘relevant place’ when not wearing such a covering. Under Paragraph 9, a ‘relevant person’ is a police constable, community support officer, Transport for London officer or person designated by the Secretary of State for the purpose of these regulations. Under Schedule 1, a ‘relevant place’ is defined as an enclosed shop, shopping centre (but not a seated bar or cafe within it), bank, post office or transport hub. If we refuse such direction by a relevant person, under Regulation 5 a constable can remove us from such a place using reasonable force. Under Regulation 6, refusing, obstructing or otherwise resisting such powers is an offence that under Regulation 7 is punishable by a fixed penalty notice of £100, which, again, may only be issued by a relevant person. Under Regulation 9, these Regulations must be reviewed by the Secretary of State within 6 months of them coming into force; and under Regulation 10 they will expire in 12 months. None of these powers are granted to an owner, manager or member of staff of a relevant place. Indeed, the Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) Regulations 2020 have nothing to do with the owners, managers or staff of the relevant places they designate. They merely extend the powers of police constables, community support officers, Transport for London officers or other relevant persons over us when in such places.
There are several things to be said about these new Regulations. The first is that — like those preceding them — they exclude the shop, bank, post-office, supermarket and shopping-centre staff, public transport employees, community support officers and police constables that are the most constant human presence in these designated ‘relevant places’ and are therefore — if we are to believe the Secretary of State for Health and Social Care — the primary source for the spread of the ‘serious and imminent threat’ the places in which they work are supposed to present. Emergency responders, too, are also exempt. In addition to these exempt persons, the following places are also excluded from the list of relevant places: restaurants with table service, hotel dining rooms, members’ clubs, bars and public houses; public libraries and reading rooms; premises providing professional, legal and financial services; premises providing medical services; veterinary services; cinemas, theatres, nightclubs, dance, bingo, concert, exhibition and other public halls; conference and exhibition centres; fitness and dance studios, indoor gyms, leisure centres, indoor swimming pools, water parks, bowling alleys, funfairs, theme parks, amusement arcades, indoor soft-play areas, skating rinks or other indoor premises for indoor sports, leisure, adventure or recreation activities; indoor sports arenas or stadia; casinos, hotels and hostels; spas, nail, beauty and hair salons and barbers; tattoo, piercing and massage parlours; storage and distribution centres; funeral directors; photography studios; and auction houses. Quite evidently, therefore, by the sheer number of public places excluded from these Regulations, they have other motivations than protecting ‘public health’.
The second thing to say is that, although they can be ignored by the owners, managers and staff of the places they designate as relevant to them, these Regulations rely for their implementation not on the various UK police forces — which have admitted that they do not have the constables to police them — but on the owners and managers of shops, supermarkets and other ‘relevant places’. However, since their staff do not have the legal powers to detain a customer who refuses to wear a face covering on the premises, or even to deny us entry to the premises under the powers conferred by these Regulations, staff can only make wearing one a condition of entry on the grounds that the premises are private property. This is what the Secretary of State referred to when he told Parliament that refusing entry would be ‘in line with how shops would normally manage their customers’. As long as doing so does not discriminate against someone under the Equality Act 2010 — that is, because of our age, race, religion, gender, sexuality, etc — staff can already refuse to serve us, and sometimes do so if, for example, we are drunk, or abusive or threatening. The new Regulations have added nothing to an owner’s rights over their private property.
What is being presented as a public measure, therefore, will in practice cause further reduction of our public rights of way over private land. This will inevitably lead, at least initially, to increased confrontation and civil disturbance in retail outlets and shopping centres. In the same way, therefore, that more and more private land in the UK is being guarded by private security guards, so too more shops — and not just shopping centres, supermarkets and banks — will employ security guards to enforce this condition. Behind the bogus reason of protecting the public from the spread of a disease that has all but left these isles, these Regulations are using the private sector to bear the financial burden of increasing the number of security guards in our public life, thereby expanding the UK surveillance state.
In the UK today, security guards, as a matter of course, wear uniforms as close as is legally permissible to police constables, often with chequered hat bands, high-visibility jackets, dark-blue clothing and jack boots. Given the British public’s general ignorance of the laws under which we live, a direction from a private security guard is accepted as having the force of law, when in fact it has nothing of the kind. The owners of private property can impose wearing a face covering as a condition of entry into their shop, and announce this condition on a sign displayed outside the premises, and this makes entry without such a covering trespass. This, however, is only a civil offence. If the owner or his or her representatives — that is to say, the manager, staff or security guard — directs us to leave the premises, to refuse to do so would then incur a charge of aggravated trespass, which is a criminal offence under Section 68 of the Criminal Justice and Public Order Act 1994. However, only a police constable has the power to detain or arrest someone for doing so, and any private security guard who tries to do so is acting illegally.
Anyone who has been following the creeping intrusion of Government measures into the public life and social behaviour of the UK will know that it will not stop here. No sooner had the Regulations making face coverings on public transport mandatory come into effect than it was announced that the Government was considering imposing the same in shops and supermarkets. The ink on the Regulations imposing the latter has not dried and already the Government has announced it is looking at enforcing the wearing of gloves to combat the spread of the virus. No one should be in doubt that the Government’s aim is to make the wearing of masks and anything else they can dream up mandatory in all public places.
Unfortunately, for the overwhelming majority of the UK public a sign outside announcing the wearing of a face covering as a condition of entry, the presence of a private security guard on the door, and the vague awareness of Government Regulations to this effect, will most likely be enough to ensure widespread compliance. The English don’t do rebellion, except when it comes to football. More effective than all these measures, though, will be the self-policing on which the UK biosecurity state has relied for its implementation since the coronavirus crisis was declared. In England, at least, if less so in Wales, Scotland and Northern Ireland, the public ‘shaming’ to which the Chief of the Metropolitan Police Force referred in her interview should not be underestimated as a method of public compliance. As Twitter has tested, demonstrated and confirmed, the shaming of deviations from social orthodoxy is one of the most powerful political tools in this most obedient and ashamed of countries. The uncovered face will become the source of a shame every bit as effective for our new socio-political order as clothing is to our naked bodies. Social media is awash with the argument that, just as under existing obscenity laws we cannot enter a shop naked, so now we cannot enter a shop without our face covered. In our radically conservative times, obedience to public shaming is presented as a measure of progress. Whatever unsubstantiated or marginal medical reasons there may be behind the prohibition are no longer relevant. The time for arguing with authority is over. A covered face in public is now the new normal.
Before it becomes so, however, we should remember that there is nothing in the new Regulations compelling or empowering staff, managers or owners of a shop, shopping centre, bank or post office to enforce the wearing of a face covering as a condition of entry or service, and remind them of the fact. Like their equivalents in the pubs, bars, restaurants, cafés and other public premises instructed by the Government to collect customers’ private details as a condition of entry or service, those who do so have chosen to police the public beyond what is required by law. Most of the pubs I have visited in London since the Government Guidance on contact tracing was issued had a sign outside saying something like: ‘In compliance with Government instructions, we can only serve you if you hand over your contact details’. This is legally incorrect, and around half of the staff I informed that it was, and showed the text of the Guidance clearly stating that it was a voluntary programme, served me without taking my details. The other half, however, refused. But whether it’s out of ignorance or choice, indifference or obedience, shame or duty, those who police the public beyond the requirements of the law are the willing instruments of the biosecurity state.
The argument for blanket masking remains the same as it was for their mandating on transport or in shops: that no matter how small the difference face coverings make, no matter how marginal their benefits, if they can save even one life they should be made mandatory. Even were it true, this is a purely medical argument, and as such its context is limited to the care of the patient’s health. Consideration of these Regulations, however, go far beyond the limits of protecting public health; and medical practitioners are not the only people we should be consulting on their justification, proportionality, legality or impact.
First, living is dangerous to an individual’s health. Some people like to keep their sofas wrapped in the plastic in which it was delivered from the warehouse, to place coasters between their coffee cups and the coffee table, spray every surface in their home with disinfectant, want to ban smoking cigarettes, drinking alcohol, eating unhealthy foods, stop children playing conkers and all contact sports, but these are pathological reactions to the physical realities and risks of life on which the pharmaceutical, cosmetic and health-and-safety industries ruthlessly prey. It’s worth recalling that the most famous wearer of masks in public places was the pop singer, Michael Jackson, who like most billionaire celebrities considered his person to be at risk of contamination from proximity to those who bought his records, concert tickets and merchandise. If you’re rich enough to be able to do so, never leaving your house may eliminate the threat of dying in a road accident, for example, or catching a common cold, but it’s hardly conducive to a healthy life, either physically or — as Jackson demonstrated — mentally. As for an individual so for the nation, physical health must be balanced against mental, social, economic and political health. To take just one example, an immunologist can tell us whether or not outsourcing our children’s immune system to a vaccine for a respiratory disease to which they are statistically immune will have negative physiological consequences for them in the future; but hopefully we can all understand that raising them — as the Government is instructing us to — to treat their fellow human beings as a source of harm and a threat to their well-being quite clearly has the potential to create a psychological and social time-bomb for the future of the UK. So the medical argument that making the wearing of a face covering mandatory in public is justified on the grounds that it may save a life is a flawed argument that isolates the issue from its wider context.
Second, making the wearing of face coverings in public mandatory is grossly disproportionate to the threat of COVID-19 in the UK. According to estimates by the Office of National Statistics, in the week ending 19 July just 1 in 2,000 people in England, excluding those in hospitals, care homes or other institutional settings, had SARs-CoV-2. This equates to an estimated 27,700 people, with around 0.52 new infections for every 10,000 persons. According to the most recent figures, the number of deaths attributed to COVID-19 in the whole of the UK in the week ending 10 July, was 388, the lowest number of deaths attributed to COVID-19 in the last 16 weeks, and constituting just 3.9 per cent of all deaths. By comparison, in the same week 789 people — twice as many — died from a respiratory disease other than COVID-19. The total number of deaths registered in the UK in the same week was 9,919, which is 587 fewer than the average over the last five years. Over a quarter of all deaths attributed to COVID-19 were over the age of 90. Three quarter were 75 and over. All but 35 in a population of 67.8 million were over 64 years old. Indeed, last week it was revealed that there were insufficient numbers of people in the UK infected with SARs-C0V-2 to test-trial the vaccine being developed by AstraZeneca — the multinational pharmaceutical company that has signed a deal with the UK Government to produce 100 million doses of the vaccine — in collaboration with Oxford University. No-one appears to have questioned why we should require a vaccine for a virus so few of us have and which is a threat to even fever; but this, again, is an indication that the ‘severe and imminent threat’ coronavirus supposedly presents to the population of the UK is a fictional construct of our Government, given scientific legitimacy by the purchased opinion of senior medical advisors, with the collaboration of the National Health Service, and disseminated by the press and media. What this data doesn’t support is the mandatory wearing of face coverings punishable by a fine and prosecution.
Third, the proponents of mandatory face coverings occasionally ask what possible harm wearing one could do. I have yet to see any of them wait to hear an answer. The ‘debate’ on masks, if it can be called that, addresses the pros and cons of wearing one as if the Regulations making face coverings mandatory have been made in isolation from the vast number of laws being made by this Government under the cloak of the coronavirus crisis. One would think — and the noisiest promoters of masks appear to be entirely ignorant of the fact — that these Regulations are being made under normal parliamentary conditions by a Government fully accountable to the scrutiny and approval of the legislature, rather than as a distraction to the vast quantity of legislation that is tearing down and refashioning the social, juridical and political structures of the UK state. The first question to be asked in any debate about whether the wearing of masks should be made mandatory is how doing so serves the Government’s ongoing implementation of the UK biosecurity state under the cloak of this crisis. This is a question for political scientists and social activists, not medical practitioners. It is a question that, in its total absence from what debate there is in both our Parliament and our media, all of us should and must ask ourselves and each other before we obediently place the sign of our compliance to that implementation over our mouths.
The press and media have framed the Government’s delay in imposing face coverings on the populations as a sign of its indecision and incompetence; while the Government, in turn, has explained its sudden change of opinion as the response to new medical opinion and scientific advice. In truth, it is neither. When the deaths attributed to COVID-19 were sufficiently high to hold the public in the grip of a panic the media did everything to increase and spread, the Government had no need of masks. Now, when the excess deaths on which the press relied for that panic has dropped below the average over the last five years, and even the deaths of 90-year-olds attributed to COVID-19 has fallen to figures that even the most imaginative bar-charts have trouble terrifying the public with, the Government needs an easily consumed sign of the presence of what it continues to call in its legislative documents ‘a serious an imminent threat to public health’. What better sign of the universal consensus to the existence of that threat than a nation masked and muzzled? Under the silencing and shaming of dissent of which the mask is both symbolic compliance (nakedness covered) and physical enforcer (speech silenced), the Government is free to continue and expand the implementation of the UK biosecurity state.
For those who wish to resist the implementation of this new socio-political order — in which laws in violation of our human rights are made in contravention of parliamentary procedure and police commissioners call on the public to shame those individuals who fail to comply with them — as with the Regulations that preceded them, all you have to do in order to avoid being compelled to wear a covering over your face in a place relevant to these Regulations is to claim exemption. Under Regulation 4, Paragraph 1, Section a, ii, a ‘reasonable excuse’ for not wearing a face covering is that it causes ‘severe distress’. Customers may wish to quote this Regulation, or to print it out and show it to staff, managers or owners, and to explain to them that they have no obligation or right to refuse entry or service under the new Regulations. Under the Equality Act 2010, you are not obliged to identify either the nature or the cause of this distress; but, once again, should you be challenged about either, you may wish to direct the questioner to the contents of this article and those listed below.
Addendum 3. Psychological Impact of Wearing Masks on School Children
Extracts from the conclusion to a psychology report by Dr. Zenobia Storah, a clinical psychologist, in respect of Civil Proceedings by Law or Fiction.
‘It is my professional opinion that current policies intended to reduce SARS-CoV-2 transmission within Child A’s School, and their manner of implementation, are causing unintended psychological and developmental harm to young people within the school community. It is my view that there is potential for significant harms to young people’s social, emotional and cognitive development and their well-being.
‘Children across the UK are being subjected to psychological and developmental harms due to widespread adoption of Government-endorsed SARS-CoV-2 policies in schools.
‘Research has shown that social deprivation and isolation have unique effects on brain and behaviour in adolescence compared with other stages of life.’
‘Given the importance of adolescence in the developmental trajectory of human beings, and increasing knowledge about the sensitivity of the adolescent brain to environmental influences and stressors, there is real potential for far-reaching consequences. Findings from recent studies have started to confirm concerns about harm caused to children and young people by such unprecedented social policies.
‘Since March 2020, Coronavirus-related Government policy has seen schools close, children compelled to stay at home and refrain from organised sport and other activities. They have been forbidden to engage in face-to-face contact with extended family members, friends and peers. For the first time in UK history, such rules have been imposed by a government upon a whole generation of children and young people, in spite of decades of accumulated knowledge and understanding about the necessary circumstances for optimal child and adolescent development. It does not seem unreasonable, therefore, to describe this as a social experiment which has been conducted without informed consent, and without due consideration of the enormous potential for harm. The introduction of social distancing and other non-pharmaceutical interventions in schools since their reopening, and the recommendation of masking secondary-school children, has clearly not been appropriately risk assessed.
Already there is compelling evidence that children and young people have borne a disproportionate psychological burden on behalf of the nation. Research findings indicate that they are facing an unprecedented mental health crisis, the full scale of which is yet unknown. Incidence of mental health disorders in young people, which has risen sharply since 2007, appears to have escalate further since March 2020. Clinically significant mental health conditions amongst children has risen by 50% compared to three years earlier. A staggering 1 in 6 children reported behaviours and symptoms hat suggested a probable mental health condition, up from 1 in 9 in 2017. Since July 2020, children and young people in the UK have endured a further nine months of restrictions of varying degrees. It seems reasonable to assume that these experiences will have had further detrimental impact on young people’s mental health. It is increasingly evident that the [Government’s response to the] pandemic has taken a devastating toll on the mental health of the young which will impact on their lives for years to come.
‘In this context, it is arguable that, now more than ever, schools have a duty of care to young people, to safeguard and promote the healthy, normative development and emotional well-being of their students.
‘Professionals working with children are trained to hold the interest of children as paramount, and have a duty to place their needs at the forefront of all they do. The Children’s Act 2004 states that the welfare and safeguarding of children is everyone’s responsibility. The UK Government is also beholden to the UN Convention on the Rights of the Child. The four core principles of the convention are: non-discrimination; devotion to the best interests of the child; the right to life, survival, development; and respect for the view of the child.
‘It is therefore deeply disturbing that, since March 2020, the principles of this legislation and the Convention appear to have been forgotten, both by many professionals and officials with responsibility for children’s welfare, and by the UK Government itself.
‘SARS-CoV-2 policies in place both within schools and wider society, work against the manner in which child psychologists and other child professional are trained to work with and think about children and young people. Since March 2020, the Government has enforced or recommended interventions which hinder communication, lower self-esteem, increase anxiety and impair development to an extent that, if this happened in a private family, it would be considered a safeguarding issue.
‘In keeping with the principles of the Children’s Acts (1989, 2004), there is a professional obligation on the part of all people working with, or on behalf of, children (e.g. teachers, social workers, psychologists, those in local authority, public health officials, civil servants, MPs and cabinet ministers) to consider whether a plan of action does in fact place children’s rights as paramount and whether it is in their best interests.
‘In my opinion, school policy in relation to limiting SARS-CoV-2 transmission not only prevents the school from supporting Child A and their peers to “thrive” and “fulfil their potential”, but is likely to be causing them psychological harm of unknown quantity.
‘The practices at Child A’s school are similar to those introduced in most secondary schools across the country, meaning the scale of damage to children is potentially monumental. Therefore, the widespread implementation of non-risk assessed and potentially harmful policies, both now and in the future, is an urgent matter for all concerned with the welfare of children and young people.’
Postscript. Summary of Amendements to the Coronavirus-justified Regulations on Wearing Face Coverings
Since 23 July, the following Statutory Instruments relating to the enforcement of face coverings have been made into law:
7 August: Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) (Amendment) Regulations 2020. These Regulations require members of the public to wear face coverings in additional indoor premises in England.
21 August: Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) (Amendment) (No. 2) Regulations 2020. These extended and clarified the scope of these Regulations by specifying further indoor premises where face coverings must be worn and additional examples of circumstances where a person would be exempt from wearing a face covering.
27 August: Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place and on Public Transport) (England) (Amendment) Regulations 2020. These Regulations increased the penalty amounts for fixed penalty notices issued under legislation governing the wearing of face coverings on public transport and in relevant places.
22 September: Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place and on Public Transport) (England) (Amendment) (No. 2) Regulations 2020. These extended the existing requirement to wear a face covering on public transport to those travelling in taxis and private hire vehicles.
23 September: Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place and on Public Transport) (England) (Amendment) (No. 3) Regulations 2020. These amended existing Regulations to require members of the public to wear face coverings in additional indoor premises in England, require the wearing of a face covering by staff or other workers working in certain retail, hospitality and leisure settings, and further increased the amount of a fixed penalty notice which can be issued for each offence.
24 September: Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) (Amendment) (No. 3) Regulations 2020. These amended existing Regulations in order to extend the scope of the requirement to wear a face covering to staff working in indoor public areas of relevant places, and where they come or are likely come into contact with members of the public, specifically public houses.
5 March: Health Protection (Coronavirus) (Wearing of Face Coverings in a Relevant Place and Restrictions: All Tiers) (England) (Amendment) Regulations 2021. These amended existing Regulations to remove the requirement to wear a face covering in polling stations for elections and referendums.
30 November: The Health Protection (Coronavirus, Wearing of Face Coverings) (England) Regulations 2021. These reimposed the requirement to wear a face covering in shops, shopping centres, banks, building societies, post offices, during driving tests, restaurants, cafes, bars, public houses, photography studios, clinics, dentists and public transport.
Simon Elmer
Architects for Social Housing
Further reading by the same author:
The Impact of Lockdown on UK Housing
In Our Defence: Freedom of Speech in the UK Biosecurity State
Behind the Mask, the Conspiracy!
Cui Bono? The COVID-19 ‘Conspiracy’
Lies, Damned Lies and Statistics: Manufacturing the Crisis
Our Default State: Compulsory Vaccination for COVID-19 and Human Rights Law
Bowling for Pfizer: Who’s Behind the BioNTech Vaccine?
Bread and Circuses: Who’s Behind the Oxford Vaccine for COVID-19?
The Betrayal of the Clerks: UK Intellectuals in the Service of the Biosecurity State
When the House Burns: Giorgio Agamben on the Coronavirus Crisis
The Infection of Science by Politics: A Nobel Laureate and Biophysicist on the Coronavirus Crisis
The New Normal: What is the UK Biosecurity State? (Part 2. Normalising Fear)
The New Normal: What is the UK Biosecurity State? (Part 1. Programmes and Regulations)
Lockdown: Collateral Damage in the War on COVID-19
Manufacturing Consensus: The Registering of COVID-19 Deaths in the UK
Giorgio Agamben and the Bio-Politics of COVID-19
Good Morning, Coronazombies! Diary of a Bio-political Crisis Event
Coronazombies! Infection and Denial in the United Kingdom
Language is a Virus: SARs-CoV-2 and the Science of Political Control
Sociology of a Disease: Age, Class and Mortality in the Coronavirus Pandemic
Architects for Social Housing is a Community Interest Company (no. 10383452). Although we occasionally receive minimal fees for our design work, the majority of what we do is unpaid and we have no source of public funding. If you would like to support our work financially, please make a donation through PayPal:


I so agree with you Adrian White! I have written to my MP about this twice, the first time I did not receive a reply, the second time I insisted on seeing the scientific data to support the Government stance and all I got back was really suspect studies and that my MP (Labour MP) agreed with the Gov. What the hell is going on, what are the journalists and entire media doing? They can’t all have the same opinions on this subject that threatens our whole way of life! I’ve seen today a video of a care home staff who say that there is a DNR policy in some care homes and that medication and food is being deprived to some elderly people (along the lines, but worse than the discredited Liverpool Pathway Care). Back then the Guardian, BBC et al were all up in arms about it – but nothing is getting through the media now – closed ranks! The FEAR is being ramped up in the public’s eye to accept all of this.
LikeLike
Hello Jennifer, you might be interested in my new book, The Road to Fascism: For a Critique of the Global Biosecurity State, which I’ve been working on since February this year and published today. It’s available as a print-on-demand book in hardback and paperback editions (with an e-book forthcoming). Please click on this link for the contents page, my preface and purchase options. Best wishes. https://architectsforsocialhousing.co.uk/2022/09/28/the-road-to-fascism-for-a-critique-of-the-global-biosecurity-state/
LikeLike
A superb and very well researched article. Do you know what grounds we can state for not wearing a mask – e.g. the Human Rights Act, or a law related to health? There must be some way of legally protesting our right not to wear a mask.
LikeLike
Hello Maya, if you want to claim exemption you merely have to state that you have exemption. I’ve done that to every shopkeeper who has asked me, and they generally accept this statement without question. To those who have asked exemption for what, I answer that they do not, legally, have the right to ask that (as it may involved a disability, etc.). If someone starts getting pushy, my answer is that I claim it under Exemption ii, Section A, Paragraph 1, Regulation 4 of the The Health Protection (Coronavirus, Wearing of Face Coverings in a Relevant Place) (England) Regulations 2020. That will shut 99% of thre busybodies up. For the 1% who asks what exemption ii is, my answer is to ask why they are enacting regulations they do not understand. The exemption is that wearing a mask causes ‘severe distress’, but that’s no-one’s business, and you have no legal obligation to inform anyone of the fact.
If, however, you mean how do we protest against these medically unjustified, wildly disproportionate and democratically unscrutinised and unapproved regulations, hopefully my articles will provide some of the arguments for not complying. Doing so beyond individual acts of non-compliance, however, and forming a movement of civil disobedience and resistance, is something that will only be accomplished collectively and through action as well as words.
LikeLike
Hello Maya, you might be interested in my new book, The Road to Fascism: For a Critique of the Global Biosecurity State, which I’ve been working on since February this year and published today. It’s available as a print-on-demand book in hardback and paperback editions (with an e-book forthcoming). Please click on this link for the contents page, my preface and purchase options. Best wishes. https://architectsforsocialhousing.co.uk/2022/09/28/the-road-to-fascism-for-a-critique-of-the-global-biosecurity-state/
LikeLike
Agree with you, Jennifer. The on-message “closed ranks” you describe are absolutely intrinsic to ‘normalizing’ muzzles.
The only objections ever allowed to seep through cracks in the grand consensus are from the eccentric usuals like Peter Hitchens, Julie Burchill, Claire Fox and a few duck-house Tory nutters waving their spats in indignation – none of whom need be considered a threat to the One True Religion 2020. Look for any discussion of the social consequences and you get bugger-all.
I wrote to my MP too (Barry Gardiner Lab), got an automated non-response. Wotta surprise.
Today I’ve called various museums and galleries with ‘enquiries’ (ha ha) – they’re all on the same script.
It gets worse dept:
Anyone read about the school including dear little face-masks as part of the uniform?
https://www.cheshire-live.co.uk/news/chester-cheshire-news/masks-become-part-holmes-chapel-18717883
The fucking things willl bear the school’s insignia apparently. Mankind may depend on kids trashing them instantly. . .
LikeLike
I am grateful to ASH for drawing to my attention John Hardie’s article ‘Why Face Masks Don’t Work’ and have made a copy of it in case our Government, the proclaimed upholder of a free society, causes it to disappear from the internet.
The gist of it is that whereas, when masks were introduced for surgeons and other medical practitioners in the late nineteenth century, only particles greater than 5 microns (droplets) could be detected, it is now known that infectious people exhale particles many times smaller, and that these escape round the edges of the best fitting mask.
For me an important question remains unanswered. We were told that in the early weeks of the coronavirus epidemic doctors and nurses were dying because they did not have the PPE; but now they have the PPE, they are no longer dying. Is it the case that something other than the PPE is protecting them? or that some other part of the PPE than the mask is protecting them? or that whereas their medical masks are good, those the public are forced to wear are not?
LikeLike
Adrian, prompted by your reference to the John Hardie article which I may’ve seen courtesy of this site (or at least got the gist of), I see it’s indeed now been ‘removed’ from the Oral Health Group website, with the following statement:
“If you are looking for “Why Face Masks Don’t Work: A Revealing Review” by John Hardie, BDS, MSc, PhD, FRCDC, it has been removed. The content was published in 2016 and is no longer relevant in our current climate.”
Whether the piece lurks somewhere online I don’t know. Papers by Louis Pasteur, much of which must have been superseded by research since the 19th century, are available for anyone to read.
LikeLike
Hello Jess, I mentioned in my quotation from the John Hardie article that it has been removed from Oral Health (18 October, 2016), but you can access it here: https://web.archive.org/web/20200509230932/https://www.oralhealthgroup.com/features/face-masks-dont-work-revealing-review/
LikeLike
You can also find it here:
https://eumeswill.wordpress.com/2020/07/09/why-face-masks-dont-work-a-revealing-review/
LikeLike
Hi. Fantastic article and comments – we must defend our democracy. Go to London Transport website, click on ‘face coverings’ and then ‘face covering exemption card’. You will see several reasons for exemption and the one that applies to those of us defending the Human Rights Act is: “Putting on, wearing or removing a face covering would cause you severe distress”. The decision is yours – you don’t need a doctor, psychiatrist or anyone else. Cheers in solidarity. John
LikeLike
Hello John, you might be interested in my new book, The Road to Fascism: For a Critique of the Global Biosecurity State, which I’ve been working on since February this year and published today. It’s available as a print-on-demand book in hardback and paperback editions (with an e-book forthcoming). Please click on this link for the contents page, my preface and purchase options. Best wishes. https://architectsforsocialhousing.co.uk/2022/09/28/the-road-to-fascism-for-a-critique-of-the-global-biosecurity-state/
LikeLike
I’ve got lots of parents freaking out that ‘public health officers’ have powers to remove children from school if they either test positive or have ‘relevant symptoms’, and can do so without notifying the parents. Is this true and do they actually have legal powers to do so?
LikeLike
about time Someone with the £ to do so, took this lot to court publicly and had it ALL thrown out, Just like johnson suspension of parliament was
LikeLike
They have, Simon Dolan and he lost.
LikeLike
Simon Dolan has appealed and its going through. Mx
LikeLike
On 2020-08-25 12:23, Charles Macmillan wrote:
Good afternoon Chris,
Contrary to the information posted on you web page:
“Due to recent events regarding the Coronavirus Disease (COVID-19) and in order to keep our staff and customers safe, we have decided to temporarily close the retail shops until further notice.”
I have received a complaint which alleges there is a sign above the door shop reading – “We Do Not Muzzle Our Customers – Mask Free zone.” This in contravention of Governments legislation:
In England, you must wear a face covering in the following indoor settings (a list of examples for each is included in the brackets):
public transport (aeroplanes, trains, trams and buses)
transport hubs (airports, rail and tram stations and terminals, maritime ports and terminals, bus and coach stations and terminals)
shops and supermarkets (places which offer goods or services for retail sale or hire)
shopping centres (malls and indoor markets)
· auction houses.
It is vital we all play our part in prevention the spread of infection. Contact me directly advising if you are in fact trading and the existence of the sign in the shop door.
Yours sincerely,
cid:image001.jpg@01D4EDE4.6562D7D0
Charles Macmillan
Environmental Health Officer
Communities
T. 01202 261714
charles.macmillan@bcpcouncil.gov.uk
bcpcouncil.gov.uk
MY RESPONSE TO THE COUNCIL…
Thank you for your email informing me that we have had a complaint. We have not received anything or had any comments from anyone so this has come as a bit of a shock.
The information on the website does not say that we are closed, in fact it states:
In order to keep our staff and customers safe, we are maintaining a social distancing policy, and where necessary, a “one-in, one-out” policy.
We also have floor markers by the shop entrance informing customers that we are operating a 2 meter social distancing policy. This is to play my part in the prevention of the spread., however it is difficult / illegal to physically force people to move in a certain way or to keep their distance from each other. It is partly their responsibility to look after their own health.
I could complain too about a number of other shops that do not practice their ‘Covid’ policy. Lidl for example have closed their tills, and just operate self service where it is impossible to socially distance. They don’t even clean the buttons between each use for example. I don’t see you challenging the big boys.
There is no law forcing people to wear masks. There is no evidence that they even work, in fact quite the contrary. Many of my staff and customers have exemptions from wearing them anyway, due to hidden disabilities such as Autism and COPD, again reasons that are no one else’s business, other than that of our doctors.
I warn people that this is a mask free zone because both myself and my sister who run the shop are exempt from wearing them. As are all shop staff that I have encountered in retail shops elsewhere. This sign is to warn people that there may be some people in our shop not wearing one. My sister is also partially deaf and relies on lip reading, and so often has to ask customers to remove their mask so that they can be understood better. This was advice given by Hidden Disabilities, and also the government website offers a badge to display asking people to remove the mask (attached)
https://www.gov.uk/government/publications/face-coverings-when-to-wear-one-and-how-to-make-your-own
I could put this poster up from the government that asks people to remove their mask so we can understand what is being said. I don’t see the difference warning people that the store is a predominately a mask free zone, to asking them to remove their masks.
Entry to our shop is voluntary. It is private property. We were deemed a non-essential shop by the government during the ‘crisis’ and were ordered to close, all the time Wilkinson were open selling soaps, candles and incense too.
If customers feel that my shop is too dangerous because of a lack of floor stickers, or the fact that I warn customers before hand that not all staff or customers are wearing masks due to exemption reasons, then they do not need to enter, they can order online.
It appears to me that the Council have lost their minds, and are living in a world of fear. I do not allow myself to be controlled by fear and will continue to use common sense, which is no longer common.
I cannot keep everyone happy either, complaints happen. If you could however forward this complaint on to me I would appreciate it. I cannot believe in the alleged complaint or even address the nature of the complaint without reading it.
The vast majority of my customers are extremely happy with my store policy, and they are aware that they have their own choice regarding their own health matters. I’m getting a lot of respect from the community regarding my no nonsense, common sense approach to fighting this problem.
I appreciate your concerns over this virus, and I would like to reassert the fact that I am playing my part in the prevention the spread of infection. I am also a responsible retailer, unlike many others who seem to get overlooked, child labour etc.
I have had no outbreaks in my shop. I will not be accused of putting lives in danger. Hand sanitizer is available for free use should people want to destroy their own natural bio immunity.
Perhaps the governments message has been a little confusing to people. If however you require any further clarification from me, then please do not hesitate to get in touch.
Kind regards
Chris Kettle
LikeLike
Amazing response. You certainly pi**ed on his bonfire.
LikeLike
Your reply was a script of genius and inspiration! Well done.
LikeLike
Good for you. I, for one, would make a beeline for your shop if I lived locally!
LikeLike
Spot on well done. I ask a question to the know all above who says its mandatory. How can anyone tell a person has a “HIDDEN” disability. This ludicrous decree is self defeating in that manner.
LikeLike
Hello Chris, you might be interested in my new book, The Road to Fascism: For a Critique of the Global Biosecurity State, which I’ve been working on since February this year and published today. It’s available as a print-on-demand book in hardback and paperback editions (with an e-book forthcoming). Please click on this link for the contents page, my preface and purchase options. Best wishes. https://architectsforsocialhousing.co.uk/2022/09/28/the-road-to-fascism-for-a-critique-of-the-global-biosecurity-state/
LikeLike
Thankyou, this is wonderful information. I hope and trust it inspires people to stand up for their rights.
LikeLike
Hello Pat, you might be interested in my new book, The Road to Fascism: For a Critique of the Global Biosecurity State, which I’ve been working on since February this year and published today. It’s available as a print-on-demand book in hardback and paperback editions (with an e-book forthcoming). Please click on this link for the contents page, my preface and purchase options. Best wishes. https://architectsforsocialhousing.co.uk/2022/09/28/the-road-to-fascism-for-a-critique-of-the-global-biosecurity-state/
LikeLike
So informative. I’ve been saying this from the start, it’s good to see all the information in one place. Thank you.
LikeLike
A recent Peer reviewed Paper
Will Evidence Based Medicine be Another Casualty of Covid-19?
Concludes ” We stand to be corrected and reserve the right to be wrong but we are united in one conclusion: the mainstays of the current interventions against COVID-19 – wearing facemasks and full economic lockdowns – which are prevalent across much of the world, are simply not based on evidence.”
https://onlinelibrary.wiley.com/doi/epdf/10.1111/jan.14543
BBC Medical Correspondent Deborah Cohen’s tweet in July 2020 should tell you all you need to know.
“We had been told by various sources WHO committee reviewing the evidence had not backed masks but they recommended them due to political lobbying. This point was put to WHO who did not deny”
LikeLike
Regulation 2020, No. 592 exempts those with a ‘reasonable excuse’ from wearing a mask on public transport and defines such excuses in a list that includes ‘it being reasonably necessary….to eat or drink.’ Yet the train companies in their notices and announcements make no mention of this and simply command passengers to wear a mask ‘at all times’ except those who are exempt. This command seems to apply to those who are exempt throughout the whole journey, such as asthmatics, but must surely apply to those who are temporarily exempt, such as eaters and drinkers. However, it may be that some uncited by-law has been passed that forbids eating and drinking. Does anyone know?
LikeLike
Totalitarian demands by definition ignore an individual’s situation but Transport for London’s online muzzling advice does still (Sept 14) include this in its list of exemptions:
“[ If ] you need to eat, drink, or take medication you can remove your face covering.”
LikeLike
Hi. I’m writing from the future. It’s March 2021. Everyone almost everywhere wears a mask. Kids at schools are told to wear masks. I wanted to ask if much have changed from time of writing your article. Are there as my new laws that would null your advices. Great article by the way.
Thank you.
LikeLike
As of last week the CDC all but admitted in a recent paper they published that masks have very or no effect whatsoever. We need to concentrate on ‘the vaccine’ (medical device) as this has been their goal from day one and is much more deadly. See the Vaxxed films on Rumble and a plethora of real scientific evidence by real courageous doctors etc online.
LikeLike
Hello John, you might be interested in my new book, The Road to Fascism: For a Critique of the Global Biosecurity State, which I’ve been working on since February this year and published today. It’s available as a print-on-demand book in hardback and paperback editions (with an e-book forthcoming). Please click on this link for the contents page, my preface and purchase options. Best wishes. https://architectsforsocialhousing.co.uk/2022/09/28/the-road-to-fascism-for-a-critique-of-the-global-biosecurity-state/
LikeLike